The Gut-Brain Crosstalk
Dr. Juni Banerjee, PhD; Neucrad Health Desk; April 3, 2021
The human gastrointestinal tract (GIT) or the gut is sterile at the time of birth. Following birth, there is an onset of microbiota i.e. a heterogeneous assembly of microorganisms like bacteria, viruses, protozoa, fungi. Interestingly, the human gut is the largest reservoir of microorganisms in the whole body and is essential for several important physiological processes including communication with the big brain. The human gut has also a second little brain called the enteric nervous system (ENS) that communicates with our big brain. Research works have demonstrated bi-directional crosstalk going on between the gut and the brain. Let’s try to understand the crosstalk of the Gut-Brain through this article.
How does the Gut communicate with the Brain?
Scientific studies have proved that gut microbiota and ENS exert its profound effect on the brain in the following ways:
- The ENS is capable of triggering big emotional changes in persons who are dealing with irritable bowel syndrome (IBS), constipation, diarrhea, bloating, pain, and stomach upset-like issues.
- Irritation in the gastrointestinal system sends signals to the central nervous system (CNS) and can trigger mood changes.
- The gut microbes constantly communicate with the brain through neural, hormonal, and immune pathways.
- The gut microbiome influences the host’s metabolism, including the metabolism of neurotransmitters (crucial for neuronal communications).
- The gut microbiota produces several neuroactive compounds which can modulate neuronal functions as well as neuronal plasticity.
- The gut microbiota can influence the hypothalamic-pituitary-adrenal axis (HPA axis) and therefore, can regulate the host’s stress responsivity. Importantly, elevated stress can lead to anxiety and depression.
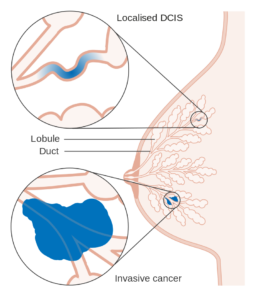
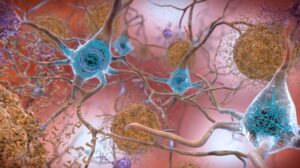
- The gut microbes are one of the key responsible factors for several mental disorders and diseases viz. Multiple Sclerosis, Alzheimer’s disease, and Parkinson’s disease.
- Alterations in the brain-gut microbiota homeostasis can worsen the pathogenesis and progression of some brain disorders and diseases.
- Rodent-based studies have indicated that gut microbiota can influence the development of its host’s emotional circuit, stress-modulation system, and pain-modulation system.
- The gut’s microbial metabolites have influences on the brain’s inflammatory processes, immune system homeostasis, and the structure/function of the blood-brain barrier.
- The gut microbiome can interact with the host cells through mitochondrial activities and microbiota dysbiosis can augment the ROS-mediated oxidative stress levels. Importantly, neurodegenerations are mostly caused by neuronal inflammations due to Reactive Oxygen Species (ROS)-mediated oxidative stress.
How does the Brain Influence the Human Gut?
We might be familiar with the feelings of “Butterflies in the stomach” as well as feelings of gut discomforts before a public-seminar/office-presentation/exam. The brain exerts profound effects on the human gut in the following ways:
- Scientists have shown that alterations in cognition, emotion, behavior, and nociception (pain) can cause abnormal gut functions leading to increased levels of inflammatory cells/intestinal dysbiosis.
- Various neuro-pathologies involving brain lesions can bring changes in the gut microbiota.
- The Enteric Nervous System (ENS) is comprised of 100 million neurons lining the gastrointestinal tract and is called the ‘brain in the gut’ or simply ’second brain’. ENS may be unable to think but is very much able to communicate back and forth with the big brain, CNS, and Sympathetic nervous systems.
- The ENS controls the process of digestion starts from swallowing, the release of enzymes required for breaking down the food, secretion of gastric acids, the release of gut hormones, peristalsis to even the blood flow involved with nutrient absorption and elimination.
- Enteric neurons cause reflexive stimulation of muscles of the gut as well as throat and can regulate the vomiting reflexes; the vomit reflex is mediated by centers in the medulla oblongata of the big brain.
- Last but not the least; the ENS is capable of interacting with the gut’s immune system.
Therapeutic aspects of the Gut-Brain Crosstalk
The revelation of gut-brain crosstalk has revolutionized the researcher’s and medicine’s understanding of the connections between brain diseases, gut microbiota, digestion, mood, depression, anxiety, thinking abilities, bowel health, etc. According to Jay Pasricha, M.D., director of the Johns Hopkins Center for Neuro-gastroenterology, “Our two brains ‘talk’ to each other, so therapies that help one may help the other”. Henceforth, Psychological interventions like CBT (Cognitive Behavioral Therapy) may improve communications between the big brain and the gut-brain, similarly, the use of probiotics as an add-on treatment for psychiatric problems like anxiety disorders and depression has also been helpful. Some studies have even indicated that stress cortisol responses get altered by probiotics. However, extensive research in the field of the gut-brain axis is still required to achieve better, effective and successful therapies.
References:
- Martin CR, Osadchiy V, Kalani A, Mayer EA. The Brain-Gut-Microbiome Axis. Cell Mol Gastroenterol Hepatol. 2018;6(2):133-148. Published 2018 Apr 12. doi:10.1016/j.jcmgh.2018.04.003
- Galland L. The gut microbiome and the brain. J Med Food. 2014;17(12):1261-1272. doi:10.1089/jmf.2014.7000
- Sudo N. Role of gut microbiota in brain function and stress-related pathology. Biosci Microbiota Food Health. 2019;38(3):75-80. doi:10.12938/bmfh.19-006
- Mayer EA, Knight R, Mazmanian SK, Cryan JF, Tillisch K. Gut microbes and the brain: paradigm shift in neuroscience. J Neurosci. 2014;34(46):15490-15496. doi:10.1523/JNEUROSCI.3299-14.2014
- Al-Asmakh M, Anuar F, Zadjali F, Rafter J, Pettersson S. Gut microbial communities modulating brain development and function. Gut Microbes. 2012;3(4):366-373. doi:10.4161/gmic.21287
- Ochoa-Repáraz J, Kasper LH. The Second Brain: Is the Gut Microbiota a Link Between Obesity and Central Nervous System Disorders?. Curr Obes Rep. 2016;5(1):51-64. doi:10.1007/s13679-016-0191-1