Organoid Culture and Transgenic animal models: Current trends for the Basic research on Novel Coronavirus
Dr. Shuvomoy Banerjee, PhD Neucrad Health Desk, July 3, 2020
Effective Corona vaccines and specific antiviral drugs are urgently required to fight against worldwide Covid-19 pandemic. However, there is undeniable call for basic research to properly understand the characteristics, life cycle, infectious tendency and patho-physiology of this novel corona virus first in order to initiate pre-clinical trials of such life-saving drugs. Scientists usually perform In-Vitro (using primary cells and cell lines) and In-Vivo (infecting live laboratory animals with viruses) research to check the potency and effects of viruses and drugs. However, finding suitable In-vivo and In-Vitro models to conduct basic research on SARS-CoV-2 (novel coronavirus) has been quite a challenge! The main reason behind this is the unknown nature, character and infectivity of the virus. At this stage, use of Tissue culture, Organoid culture, and special animal models has gained immense response and interest to persue the ongoing basic research on SARS-CoV-2.

In-Vitro research to determine the mode of SARS-CoV-2 infection:
Notably, the novel coronavirus mainly attacks the cells of the human lungs and trachea. To underatand the reasons, we need to check the cellular physiology of Human lung cells. In particular, Primary Airway Epithelial Cells contain essential receptor proteins, Angiotensin Converting Enzyme-2 (ACE-2) and Transmembrane Serine Proteinase-2 (TMPRSS-2). During viral infection, the Spike protein (S-protein) of coronavirus binds to the cellular receptor protein while the other two enzymes allow the virus to enter into the cell. Now, scientists found conducting research with primary cells is not only expensive but incomplete as the cell cannot be cultured for long time. On the other hand, with cell lines (which can grow for infinite generations) problem lies that the Novel coronavirus infect them in very low amounts.
Scientist Jennifer Harcourt succeeded to solve the issue. He used ‘Vero’ cells (cells obtained from the kidneys of African green monkeys). Interestingly, these cells doesn’t produce the antiviral protein-Interferon (IFN) allowing the Novel coronavirus to enter the cell effortlessly and start replication. Of Note, Dr. Sutoku Matsuyama, a scientist at the National Institute of Infectious Diseases in Tokyo, Japan, generated Genetically Engineered Vero-E6 cell line where the TMPRSS-2 protein is over expressed and multiplication of coronavirus happens easily. Some concern still remain about the In-Vitro tissue culture system like there is a big difference between monitoring viral infections in cultured cells at special conditions rather than monitoring infections in various organs of human body. Henceforth, scientists have started considering organ culture to understand corona infections in a more effective way.
The remarkable yet specific 3D Organoid Culture to study coronavirus:
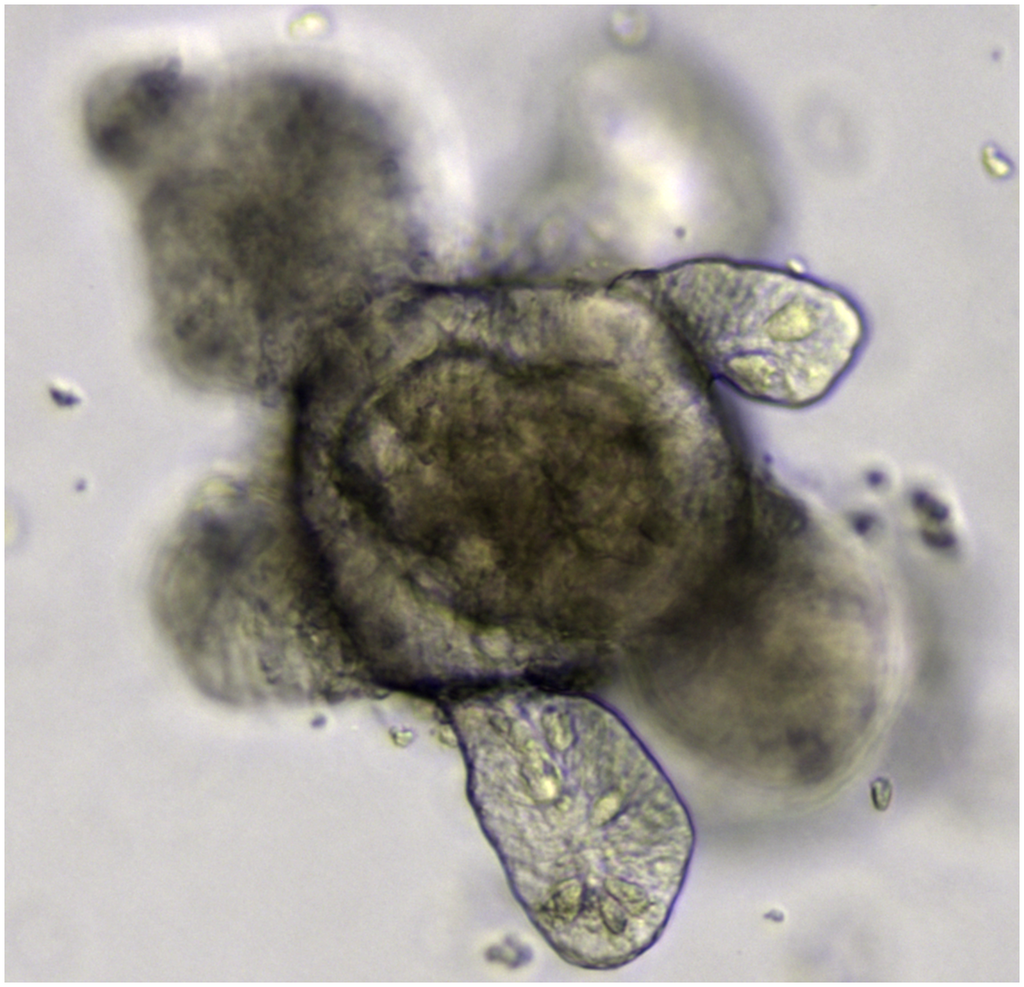
The 3-Dimensional Organoid Culture has been introduced as a modern In-Vitro model. However, before discussing this topic, let’s understand – what is ‘Organoid’? The ‘Organoid’ is a small version of the organs of human body. Scientists collect cells from specific organs via biopsy technique which can be easily cultured using special growth media and maintaining some specific and artificial physiological conditions same as tissue culture. The aggregate of cells formed as a result constantly divide to form tiny organ like structure or “Mini-Organ”. This Mini-Organ carries all the features of the main organ of the body. The production and maintenance of miniature of various organs (intestines, stomach, liver, pancreas, lungs and brain) is called ‘3-Dimensional Organoid Culture’. Recently, studies on Organoids have helped demonstrating the pathophysiology of the SARS-CoV-2 virus infection fully. Moreover, testing of antiviral drugs as a pre-clinical trial can be performed on this Organoid culture.
However, Organoids act as isolated parts of the body and corona infection spreads throughout the body via bloodstream affecting other body organs as well. Therefore, inflammatory reaction begins by over-reactive body immune system meaning it is not possible to review body’s ‘systemic response’ through Organoid culture alone! As a result, scientists have began thinking about the In-Vivo or ‘animal model’ for pursuing the Basic research on SARS-CoV-2virus.
Application of ‘Animal Model’ in Novel Coronavirus Research
To comprehend the complexity of the various stages of coronavirus infection and the pathophysiology of different affected organs in post-infective stages, it is necessary to understand the inter-relationship between the host and the virus first. For that reason, scientists heavily rely on animal models. In general, rats or ‘mouse models’ are preferred by scientists among other mammals. However, studies have shown that SARS-CoV-2 does not infect mouse at all! So, what is the way out?
Dr. Linlin Bao, a scientist at the Key Laboratory of Human Disease Comparative Medicine in Beijing, made a remarkable discovery. He found that cells in mouse do not contain ACE-2 protein, the essential factor for the coronavirus to enter into the host cell. Henceforth, by expressing human ACE-2 proteins into mice cells, Dr. Bao generated ‘Transgenic Mice’ which are easily infected by the coronavirus and showed symptoms of Covid-19 just like humans!
Currently, research is underway on Syrian hamsters who are in the same group as rodents. According to Taxonomy, Rhesus monkeys are very close to humans and hence, In-Vivo research on Primate Cynomolgus Macques and Rhesus Monkey has also started for being used in pre-clinical trials of different corona vaccine projects. Hopefully, good results have already been obtained by applying Adenovirus vector vaccine, DNA vaccine and antiviral Remdesivir drug on these rhesus monkeys.
Henceforth, Basic research work on Organoid Culture and Transgenic animal models has become inextricably linked to open the complete analytical window of understanding novel coronavirus infection biology and paving the way for corresponding drug discoveries.

References
- Takayama, Kazuo. “In Vitro and Animal Models for SARS-CoV-2 research.” Trends in pharmacological sciences, S0165-6147(20)30129-2. 30 May. 2020, doi:10.1016/j.tips.2020.05.005
- Zhou P, Yang XL, Wang XG, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020;579(7798):270-273. doi:10.1038/s41586-020-2012-7
- Matsuyama S, Nao N, Shirato K, et al. Enhanced isolation of SARS-CoV-2 by TMPRSS2-expressing cells. Proc Natl Acad Sci U S A. 2020;117(13):7001-7003. doi:10.1073/pnas.2002589117
- Ranga A, Gjorevski N, Lutolf MP. Drug discovery through stem cell-based organoid models. Adv Drug Deliv Rev. 2014;69-70:19-28. doi:10.1016/j.addr.2014.02.006
- Bao L, Deng W, Huang B, et al. The pathogenicity of SARS-CoV-2 in hACE2 transgenic mice [published online ahead of print, 2020 May 7]. Nature. 2020;10.1038/s41586-020-2312-y. doi:10.1038/s41586-020-2312-y